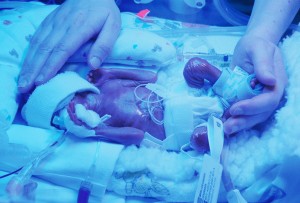
Our son Gabriel, a day after being born at 22 weeks and 6 days of gestation in 2012. He is under a bilirubin light to help break down toxins in his skin that his liver was too immature to deal with.
A new set of guidelines has come out for the resuscitation of preemies, and it means a huge deal to families such as ours. It provides more hope that preemies born in the 22nd week can get treatment.
Shortly before our son was born at 22 weeks and 6 days of gestation, the on-call neonatologist told us that they had a rule at the hospital that babies should not be resuscitated before 23 weeks and 0 days. “I don’t recommend that babies should be intubated at this stage because the results are so poor. If you give birth after midnight, I’ll be the one who comes and treats him, but my heart won’t fully be in it.” This caused us considerable stress, wondering “Is he going to show up?” He did, the birth occurred at 11:20 p.m., and he “rounded up” and saved our first and only son.
In the weeks and months after the birth, I kept thinking, “Can he really do that?” That is, refuse to treat a child when the parents want it, knowing that withholding care will result in the child’s death? Some research in to the topic revealed that yes, he can do that — a physician is not required to provide treatment that he or she views as futile.
Not only that, his recommendation was in line with the National Resuscitation Program guidelines that were in effect at that time. The birth was in 2012, and the guidelines from 2010 gave a list of conditions when it was not ethical to resuscitate:
When gestation, birth weight, or congenital anomalies are associated with almost certain early death and when unacceptably high morbidity is likely among the rare survivors, resuscitation is not indicated. Examples include extreme prematurity (gestational age <23 weeks or birth weight <400 g), anencephaly, and some major chromosomal abnormalities, such as trisomy 13 (Class IIb, LOE C).
“Not indicated” is medical-journal speak for “you probably should not do it.” The limit of viability, or the gestational age at which survival is thought to be hopeless has been steadily dropping over the past 50 years as new medical inventions including ventilators, CPAP, and surfactant replacement therapy have each made it possible for a new group of preemies to survive. Before surfactant, the limit was thought to be 28 weeks. When we checked in to the hospital with Miri’s pre-term labor, we were told that 24 weeks was the limit, and 22 weeks was just impossible.
Since 2010, however, a number of new studies have come out showing that 22 weekers have a better chance than previously thought. One found that survival rates in the United States vary wildly based on the willingness of doctors to treat. The overall survival rate of 22-week preemies was 5 percent, but if you focused only on the babies who received treatment, the survival rate increased to 23 percent. A Japanese study found that 36 percent of 22-week preemies survived there, as did 63 percent of 23-week preemies. The Japanese have been routinely resuscitating 22 weekers since the 1990s.
Just last month (October 2015, that is) a new set of guidelines for neonatal resuscitation came out, published jointly by the American Academy of Pediatrics and the American Heart Association with a different statement on the lower limit:
If responsible physicians believe that the baby has no chance for survival, initiation of resuscitation is not an ethical treatment option and should not be offered. Examples include birth at a confirmed gestational age of less than 22 weeks’ gestation and some congenital malformations and chromosomal anomalies.
This moves the “line in the sand” back from 23 weeks and 0 days to 22 weeks and 0 days. I was also glad to see the part about “unacceptably high morbidity among the survivors” dropped. We did not think potential disability was a good reason for the doctors to refuse care.
Additionally, the guidelines put more emphasis on parental choice:
In conditions associated with a high risk of mortality or significant burden of morbidity for the baby, caregivers should allow parents to participate in decisions whether resuscitation is in their baby’s best interest. Examples include birth between 22 and 24 weeks’ gestation and some serious congenital and chromosomal anomalies.
The hospital where Gabriel was born has also since removed its “line in the sand” policy for 23 weeks and 0 days in favor of a more individual approach that looks at more factors than just gestational age, including weight. Our son was 652 grams at birth, which put him in the 97th percentile for size. This helped him survive. A doctor we talked to at a recent visit back to the hospital said that a preemie that age weighing 350 grams would have a much harder time, and the decision over whether to resuscitate the child would probably be different.
These changes mean that parents in our situation of having to decide whether to ask for resuscitation of their micropreemie will still have a heart-wrenching decision to make — do you try to save the child, or do you say that you love your child enough to let him go and not make him go through the painful treatment? It may be that the latter is the better decision. But, for parents who do want to go forward in the 22nd week, this provides important support.
