When I took our twin toddlers to their 18 month check-up, I had a list of questions for the pediatrician, one of which was, why does our daughter almost exclusively breathe through her mouth? The pediatrician took one look in her throat and said her tonsils seemed a bit large. She asked a few questions about her sleep habits (she sleeps really well, or so I thought) and suggested that we go see a pediatric ear, nose, and throat doctor (ENT). Luckily, we’re still finishing up all our appointments from our preemie days, and we already had an appointment scheduled with the ENT for one final check of our kids ears.
The ENT resident came in the room, and I explained what was going on. He asked if I ever noticed her not breathing at night, if she snored, if she ever gasped for air or wheezed while she was sleeping. I had a huge wave of mommy guilt come over me–our monitor had been broken for months, and we never had a video monitor. We did some co-sleeping in the beginning, but our kids always sleep better by themselves in their cribs. I knew we’d heard her snore a few times, but I hadn’t noticed anything else he asked me about. I couldn’t really answer his questions.
He took a look in our little one’s mouth, which took all of about 2 seconds, and exclaimed that her tonsils were quite large and by his estimate, a size 3 out of 4 (on this scale, “4” is the largest touching in the throat). The attending came in a few minutes later and confirmed his observation and suggested that we participate in a sleep study to see if our little Neala suffered from sleep apnea due to her large tonsils.
Scheduling our appointment with the sleep center was quite a process, but we were able to have an initial consultation (where the doctor again confirmed her large tonsil size) and schedule our sleep study within about three months.
I did some research before we went to the sleep study and read through all the material I was given from the sleep center, but was really not prepared for our night.
The Sleep Study (polysomnogram)
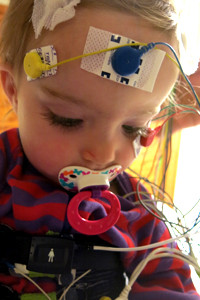
At this point, the tech was about half way done applying all the electrodes, sensors, belts, and cannula.
Our kids have always slept by themselves in a crib, and I assumed Neala would be in a crib for her study. When we arrived I was informed that we’d both be sleeping in a queen sized bed so that she could be connected to all the electrodes, wires, and other sensors and so she could be monitored by a video camera mounted above the bed. I love snuggling with our kiddos, but it’s not that fun all night long. And when they’re attached to so many wires, it’s really not fun at all.
We arrived at 8:45 as instructed, and the technician asked asked if I preferred to have Neala “hooked up” while she was awake or if I wanted to wait until she’d fallen asleep. We decided to go ahead with the application of all the stickers, belts, goo, and cannula while she was awake and she did great! She asked for her brother through the entire application process (about 45 minutes) and said over and over, “Oh cool!” when the tech put a new sticker on her!
When it was all said and done, she had around 20 wires connected to her legs, chest, face, and head. She also had a nasal cannula to sense her breathing, and it had a little antennae sticking off of it to sense if she was breathing through her mouth, and an oxygen saturation monitor attached to her toe (she hated the O2 monitor the most and lifted her foot up to see the little orange light shining under her sock multiple times during the middle of the night and then screamed in anger). There were two belts around her torso area that measured her work of breathing. The tech explained that there were sensors to monitor if she was dreaming, if she was awake or asleep, her heart rate, if her eyes were open or closed, if she was breathing, and, as mentioned above, her oxygen saturation.
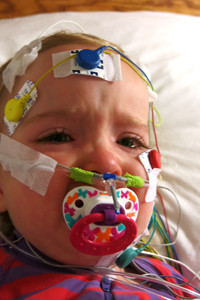
After about 45 minutes, everything was applied for the study. She really only cried for about 30 seconds…I just happened to capture this heartbreaking moment!
It was around 10:00 when we finally tried to fall asleep. Neala took much longer than her usual 5 minutes to fall asleep (I’ve been blessed with kids who fall asleep pretty quickly, thankfully), and for the first two or three hours, every time she’d move she would cry for a minute or two. The tech had to come in once to replace the sticker and wire that were stuck to her face closest to her eye. She was NOT happy with this and cried for about 10 minutes. Finally, around 2:30 A.M. we both fell into what I thought was a deep sleep. Until 5:30 A.M. when the tech came in and started ripping off the stickers, ouch. Little Neala did well with the removal and we said bye-bye to the stickers and the belts. She was clearly a bit traumatized by the whole ordeal because just this morning, weeks later, the first words out of her mouth were, “Bye bye belts, bye bye stickers.”
We celebrated the completion of the study with bacon and eggs at a local diner. I’ve never seen someone so excited about bacon!
The Results
We expected to receive the results of our test within about two weeks and had an appointment to review the results with the ENT a few weeks after that. When I received a call from the sleep center the afternoon after we’d completed the study, I was startled, to say the least. They said that because Neala’s results were so severe, they wanted to let us know. She was diagnosed with severe sleep apnea. I was terrified and again, the wave of mommy guilt hit me like a ton of bricks–how long had my kid not been breathing at night?! I weaseled my way into an appointment with the ENT at the end of that very same week (this is pretty much unheard of and I’m sure that receptionist is ready to kill me but oh well!).
When we met with the ENT, he expressed his concern regarding Neala’s apnea but also explained that she had several “events” where her oxygen saturation levels dropped into the low 80s and stayed there for up to 4 minutes at a time. After weeks in the NICU and being in and out of the hospital with our other twin all spring with respiratory issues, I knew this wasn’t good. He recommended surgery to remove her tonsils and adenoids and explained the risks and benefits. Our biggest concern was putting such a young child under anesthesia and he suggested that we weigh our options: either we have one dose of anesthesia with possible complications, or we wait until she is a bit older and risk possible developmental delays as a result of her not getting enough oxygen at night. The choice was not one we took lightly but it was clear that she needed the surgery as soon as possible.
I requested a copy of our sleep study results from the sleep center and received a 4 page document that included a written description of the results, tables of data, and a few charts and graphs. The paragraphs below are a portion of the written results (the bold text was also bold in the original document from the sleep center:
Respiratory Events: Severe Pediatric Obstructive Sleep Apnea (OSA) was demonstrated. The pediatric obstructive respiratory disturbance index (PORDI) was 14 events per hour of sleep (normal < 1.5 events/hr; mild 1.5 – 5 events/hr; moderate 5 – 10 events/hr; severe >10 events per hour). Respiratory events were more frequent during REM sleep (REM ORDI 39). Snoring was intermittent. Flattening of the nasal pressure tracing is suggestive of nasal obstruction due to mucus, nasal turbinate congestion, or adenoid hypertrophy.
Oximetry Monitoring: The average oxyhemoglobin saturation during wake was 95%. The average oxyhemoglobin saturation during sleep was 95% (95% during NREM sleep and 94% during REM sleep). Saturations were at or below 89% for 1% (4 minutes) of the total sleep time. Episodic desaturations were associated with respiratory events and were most prominent during REM sleep. The oxyhemoglobin saturation nadir was 81%.
Neala’s surgery is scheduled for late October. In the meantime we’ve been instructed to keep her nasal passages moist and clear with saline drops and to have her sleep propped up (with a pillow), run a humidifier in her room, and to try to keep her from sleeping on her back.
Practical Things to Know
- Be flexible. Our ENT typically works with a specific sleep center; however, that center did not have any openings even for an initial consult appointment for almost 6 months and they suggested another sleep center.
- If your schedule allows it, ask to be added to a list of patients to call when someone cancels last minute. I would recommend doing this for the ENT and the sleep center.
- Bring any items your child usually sleeps with. I was happy to have a blanket from home and it was very comforting to Neala.
- Bring something to distract your child while the electrodes, belts, and cannula are being attached. We had a few books that kept her entertained.
- Make sure your child is wearing pajamas that give easy access to their chest, belly, and feet. Neala wore zip up pajamas without feet and wore a sock over the oxygen saturation monitor on her left foot. Two piece pajamas would probably work well for an older child who would not try to pull the electrodes off the abdomen. Pajamas with snaps might also work well (see below regarding diaper access).
- Make sure your child has a clean diaper (if they’re still in diapers) before the technician begins attaching all the equipment. There was a moment in the middle of the night when I thought we had a poopy diaper to deal with, and I realized that there was really no way to access the diaper!
- Your child will need a shower in the morning to wash the “goo” out of their hair. In our experience, goo removal took a long time with constantly running warm water.
Have you had experience with sleep apnea or participated in a sleep study for your child?

