The following is from Hand to Hold community member Lacy. If you are interested in sharing your story, email leighann@handtohold.org.
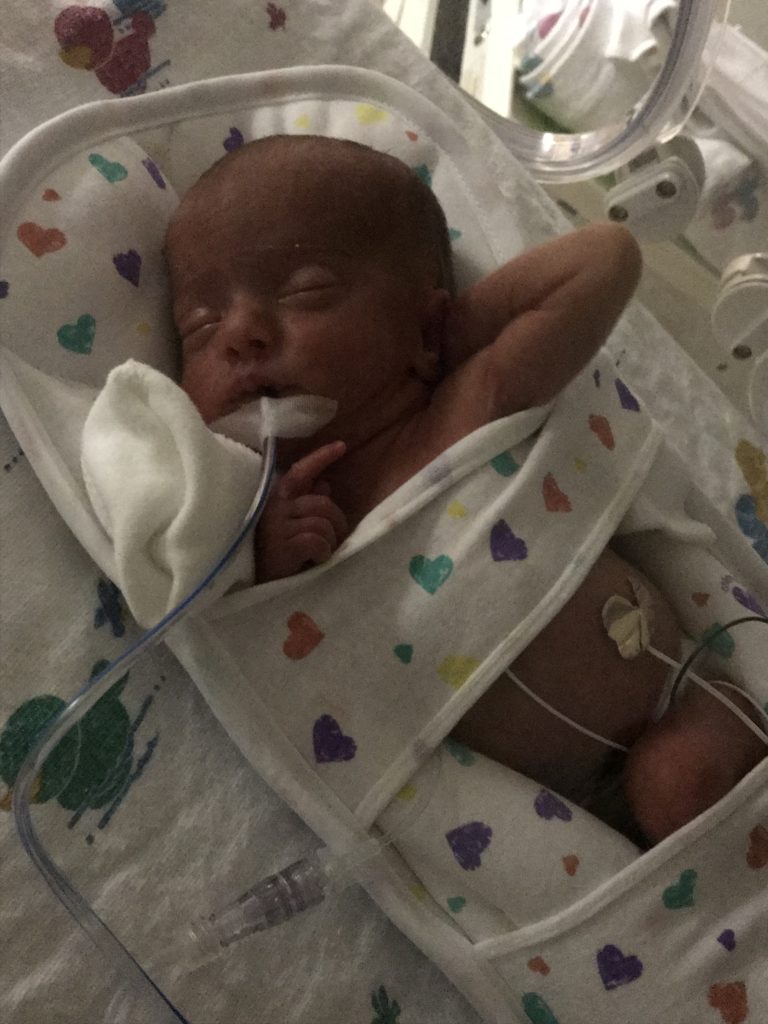
Photo courtesy of the Hale family
What were the circumstances surrounding your child’s birth?
At my 20 week anatomy ultrasound, Stevee wasn’t cooperating and the tech couldn’t get a good picture of the left side of her heart. Dr. Carl, my life saving OBGYN, didn’t see a reason that anything would be wrong with her heart and said we could check her again at 30 weeks. At the 30 week appointment, Stevee’s heart looked great, but the tech noticed two bubbles in her abdomen and that my cervix was almost gone. We were told that Stevee had duodenal atresia, a blockage of the first portion of the small intestine, and would need a surgery once she was born.
At this point, Dr. Carl put me on complete bed rest and got me in with a specialist in Dallas, Dr. Gaffney, who confirmed everything. Dr. Gaffney wanted me to deliver at Medical City Dallas, and she would get me connected with the doctors Stevee and I needed. In the meantime, they sent me to Christus Trinity Mother Frances Hospital in Tyler for observation. However, once we got to Tyler, I was having contractions that I couldn’t feel because I was retaining so much fluid.
I was admitted to the hospital and my water broke that night. Dr. Carl decided not to transfer me to Dallas, because of the risk of me going into labor. I was in the hospital for four days and then had a c-section. Stevee was transported to Medical City Children’s Hospital early the next morning, where she stayed in the NICU for 61 days.
What complications, diagnoses or surgeries did you or your child face?
Stevee weighed 3 pounds, 1 ounce. Dr. Black, her surgeon, wanted her to weigh around 4 pounds before her surgery to clear the duodenal atresia. She wasn’t on any oxygen and got her nutrition thru her PICC line (peripherally inserted central catheter). The waiting game was very hard; we wanted Stevee to be home.
Stevee underwent surgery for her duodenal atresia at about three weeks of age, and it went well. She was on the ventilator when she came out of surgery and was extubated the next day. She struggled though, so they put her back on the ventilator and then had to be re-intubated. She had a rough couple of days, but she was eventually extubated and put on a CPAP machine, then a nasal cannula. About a week later she was taken off the oxygen for good.

Photo courtesy of the Hale family
What type of support did you receive in the NICU or once you were discharged?
My family and close friends. My friend Whitney Guth, who had two babies premature, was extremely supportive and passed on lots of information. Kelli would call and check on us during our stay as well!
How old is your child now and how are they doing?
Stevee is six months old and doing wonderful! Her smile can light up a room. She loves rolling over and watching everything her older brother does!
How did your whole family cope with this experience? How are you all doing now?
There were hard times, and there were happy times. We are all doing well, just so blessed that things turned out the way they did!
What did you learn about this experience that you’d like to pass on to others?
Prenatal care is so important! Without Dr. Carl, there is no telling what could have happened to Stevee. We may have never know that she had duodenal atresia.
If you have a story you’d like to share, email leighann@handtohold.org.
