by Donna Klostermann
As I progressed through my pregnancy, I relaxed each time we passed a milestone. After I reached 36 weeks, I breathed a sigh of relief because, if my baby were born, he or she would probably survive. My attitude as I made it to 41+1 weeks was downright cavalier. I had an extremely normal, healthy pregnancy. So, as I reached my due date and proceeded to plow right through it, I thought, “I am going to go into labor, pop this kid out and be home in two days.” Although it works this way for some women, in my case, it could not have been farther from the truth.
The night my doctor scheduled my induction was the night I went into labor. I relaxed most of the day, as I was feeling quite tired. At 6:30 p.m. I called to check in before my induction. If they were full in labor in delivery, they would put me off. The nurse said they were a little full, and may call me in a couple hours. I was having cramps/contractions, but nothing out of the ordinary for being nine months pregnant.
My husband and I went to my parent’s house for dinner. At 7:00 p.m. my contractions became more regular. By 7:45 p.m. they were five minutes apart. This was going quickly, and the hospital was an hour away. Twenty minutes from home, my contractions were about two minutes apart. By the time we arrived at the hospital, my contractions were 30 seconds apart.
In triage, my baby’s heart rate was reading about half of what it should have been. I knew things were going awry. They tried to change my positioning to no avail. I was four centimeters dilated and 90% effaced. The residents tried to get a read on the baby with a vaginal heart rate monitor. They broke my water in the process and found meconium present. My contractions were not stopping. It was clear my baby was stressed, and I needed a C-section.
My doctor made it into the delivery room at lightning speed. The anesthesiologist attempted the spinal block three times before it would work. “If it doesn’t worth this time,” I told him, “put me out, cut me open, and save this baby.”
Caroline Grace Klostermann was born at 10:08 p.m., within about an hour of our arrival. I was so glad we did not find out the gender before birth, because this surprise was the only happy memory I have from this traumatic birth experience. She weighed nine pounds, one ounce, and had an APGAR score of three. I saw she was blue, and a girl. Then the resuscitation team took her away. I told my husband to go with her.
My parents went down to see Caroline before sitting in recovery with me. The neonatologist said that Caroline had lost a lot of blood and oxygen. The NICU team placed her on a ventilator because the meconium badly damaged her lungs. She was receiving a blood transfusion. She would need cooling therapy because she was without oxygen for so long and was considered hypoxic. Her chances of survival were quite small, as the neonatologists believed her organs would shut down. If she miraculously survived, she would have severe brain damage.
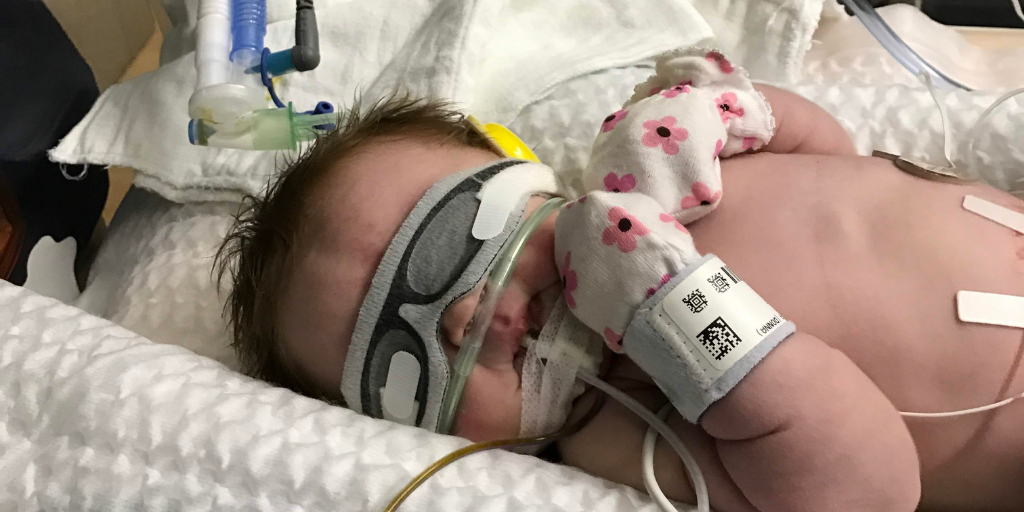
When I saw Caroline for the first time, she was hooked up to many machines, wearing earmuffs and sunglasses to reduce stimulation of her brain. Lying flat in my bed due to the spinal block, I could not really see her around the medical equipment. My nurses wheeled me back to my room to rest. Labor and delivery is an eerie place to recover without your baby.
About every 30 minutes I asked, “When can I see my baby?” They wheeled me down the next day to see her baptized, in case she did not survive. My recovery was a moot point. I did not care about myself or the pain I felt. I peed as soon as the catheter came out, regardless of how badly it hurt. I walked all up and down the halls, because each step I was closer to being with my baby. I did not want to take the pain medicine because it made me too foggy.
When Caroline was 36 hours old, she stopped responding to the ventilator and nitric oxide. It was quite literally a decision of life or death as the head of the NICU explained the risks associated with going on ECMO, and what would happen if we did not place our daughter on ECMO. ECMO, or extracorporeal membrane oxygenation, is a heart and lung bypass. This would allow the machine to breathe for her while her lungs healed. The risks included brain bleeds and death. I looked at the doctor and my husband and said, “If we don’t put her on ECMO, she will die anyway, so this is not much of a decision. “
Caroline went onto ECMO without any issues. The days were a blur of visitors, pumping and looking at my sedated newborn. When she was about three days old, I started to understand what really happened to her. I missed her dearly inside my womb. I cried myself to sleep each night because I was lonely only for her. I had a baby who I had never seen open her eyes, heard her cry, much less gotten to hold her.
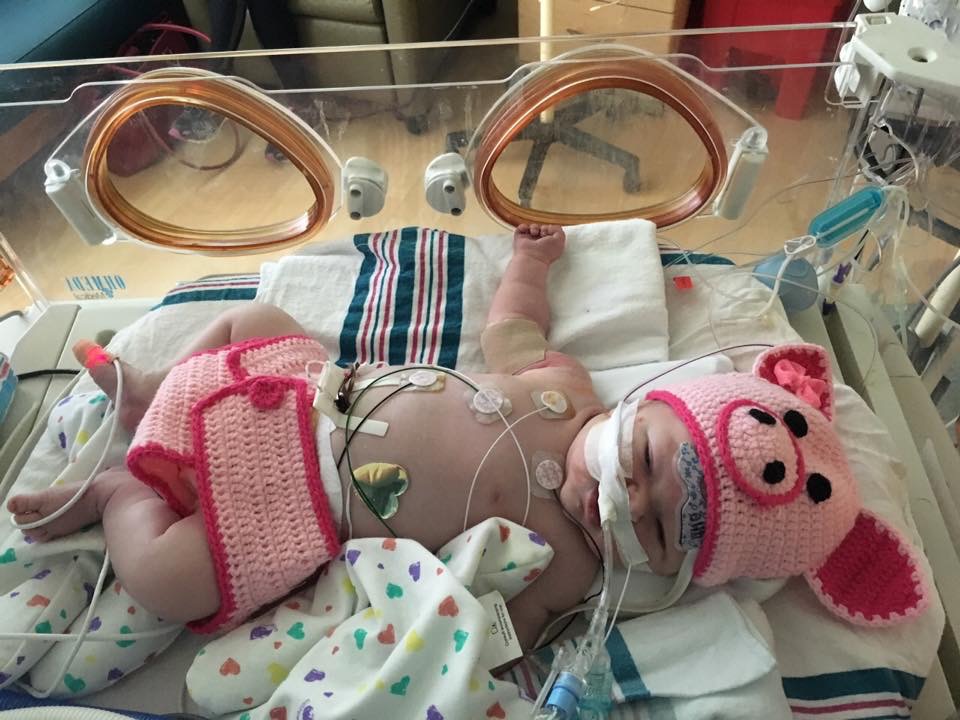
At 72 hours old, the doctors began weaning Caroline off cooling therapy. She came out of it perfectly without any seizures. After five days of ECMO, she was able to breathe through a ventilator again.
Each time Caroline had a small setback, I blamed myself. The NICU social worker and the neonatologist on duty the night Caroline was born pushed for the NICU staff to let me hold Caroline. At that point, I really needed it. At eight days old, I was finally able to hold my baby.
After holding my baby, I was elated. It was a clear sign things were going better. The NICU social worker warned me that the better Caroline got, the worse I would get. I cried for about two hours straight later that evening. I finally understood how closely I had come to losing my first child.
The next nine days were comprised of weaning off breathing support, pumping breast milk and working on feeding. At 17 days old, Caroline Grace Klostermann was able to come home from the hospital without monitors or medication. She only needed to follow up with her pediatrician on a normal basis and with neuropsychology on an annual basis. The state would follow up with Caroline through early intervention. At two months she was rolling over. At six months she crawled, and at 13 months she walked.
Caroline Grace Klostermann is nothing short of a miracle. She is a happy, strong-willed 2-year-old who loves pigs and Mickey Mouse. Other than having one vein that gets pronounced in her neck when angry (due to ECMO), she has no evidence of what happened to her. Caroline has no developmental delays and is 100% on track, if not ahead. God is great.

I still carry some emotional scars from our NICU stay. After two years, I still have nightmares. I have seen a counselor, but I waited until Caroline was five months old. I wish this was encouraged more at my NICU discharge class, instead of how to swaddle a baby. It took me failing a postpartum depression screening to realize I had NICU PTSD.
I am scared to death of getting pregnant again. I do not want to buy anyone a baby gift until after his or her baby is born, and I probably will be this way forever. I felt so alone for a long time. However, I did learn not to take childbirth for granted. It never once occurred to me during my pregnancy that I may not bring my baby home.
I discovered Hand to Hold when Caroline was six months old. The podcasts made me feel as if I was not alone. I had a happy ending, so I felt guilty expressing my feelings initially. Postpartum mental health issues need normalization, and mental health care needs to be incorporated into postpartum care. My C-section scar healed beautifully, but these emotional scars will take years to heal.
About the author
Donna Klostermann is the mom of a full-term NICU baby, Caroline, who spent 17 days in the NICU. Donna now volunteers as a Hand to Hold Peer Mentor, so she can help other parents who experience a traumatic birth and NICU stay with their baby.
