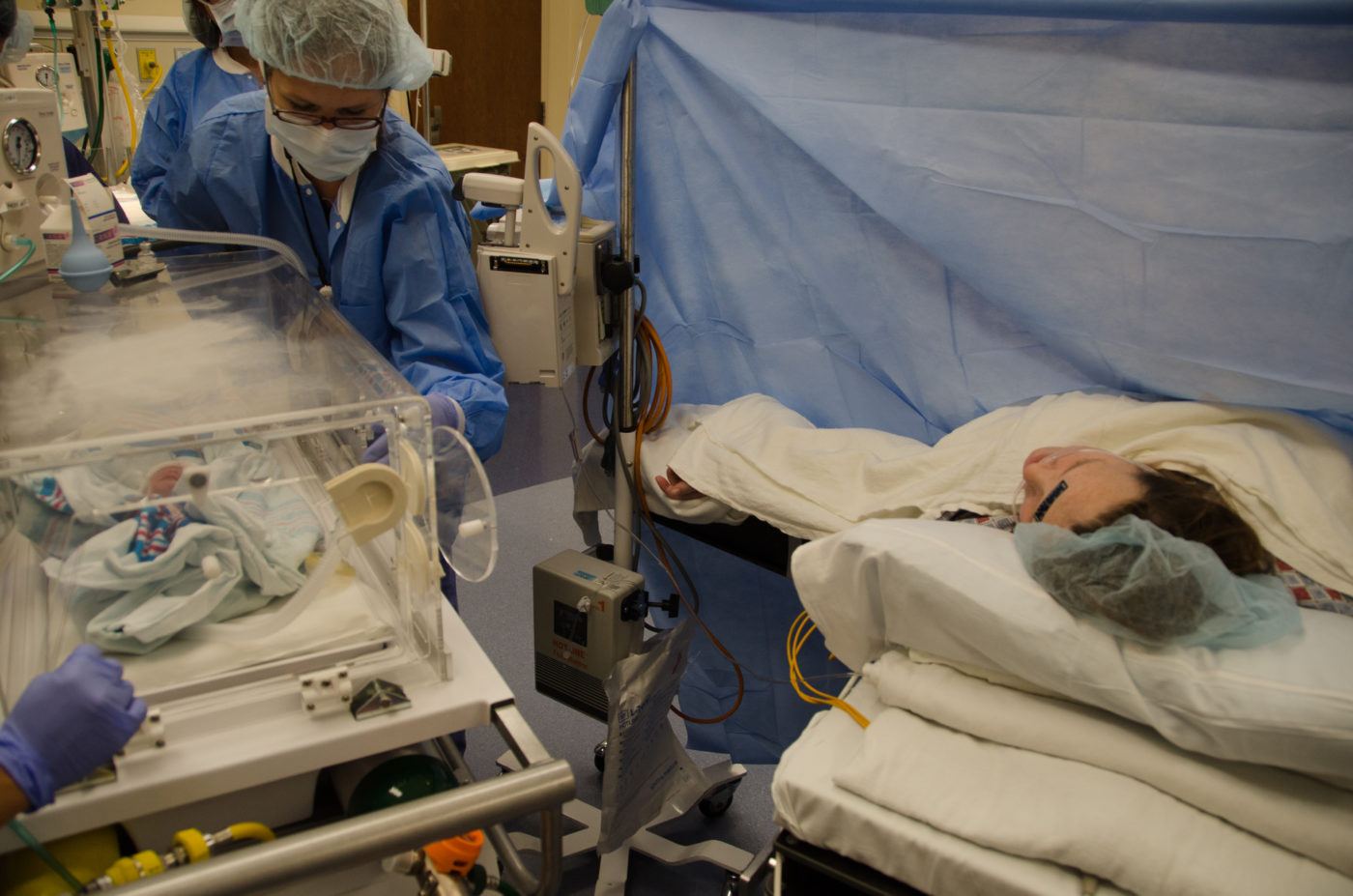
Our story
Our daughter was born at 26 weeks gestation weighing only 1lb 8oz. due to severe preeclampsia. As soon as she was born, I remember asking, “When is she coming home?” and the countdown began. Most babies come home around their due date, which in our case would be in 100 days. She fought so hard in the NICU. Her time was not easy with NEC, a stricture in her gut that caused her to need surgery, food intolerance issues, stooling issues, and excessive vomiting. At the end, it felt like it was taking so long for her to come home. It felt like maybe she never would, and my patience was running out. Even though she was still having several GI issues, I was living at the hospital (trying to bottle and breastfeed to get her home), and I felt as though at that point I could take over all the cares/struggles we were having. We had a family meeting, made sure I was trained all the enemas, suppositories, medications, and our graduation date had finally come, 114 days after she was born. We brought her home on New Year’s Eve 2015.
What I imagined vs. reality
 I imagined that when we came home, things would just continue to get better. I imagined that the worst was behind us, we survived, and now we would continue as a “typical” family with just a few things to work through and people keeping an extra eye on her while she got stronger. I was incredibly happy to have her home. My husband and I would spend hours laying with her, holding her, talking about every face she made, every little thing she did. We were smitten. Each day was a gift, each outfit was ridiculously cute, everything she did was incredible, and we were pretty sure we had the best human on the planet living in our home. We did not know how it was possible, but it was true, and she was ours.
I imagined that when we came home, things would just continue to get better. I imagined that the worst was behind us, we survived, and now we would continue as a “typical” family with just a few things to work through and people keeping an extra eye on her while she got stronger. I was incredibly happy to have her home. My husband and I would spend hours laying with her, holding her, talking about every face she made, every little thing she did. We were smitten. Each day was a gift, each outfit was ridiculously cute, everything she did was incredible, and we were pretty sure we had the best human on the planet living in our home. We did not know how it was possible, but it was true, and she was ours.
My dreams of what our home life would be like were quickly shattered and replaced with a reality of excessive projectile vomiting, blood in stool, enemas, food intolerance, sleepless nights, and a baby in pain. All the things babies do – eat, sleep, poop, repeat – she struggled with. She was sick. We quickly realized we were not out of the woods yet and had basically just entered them. Little did we know it would take years and possibly a lifetime to get through.
Isolation
We brought Adeline home smack dab in the middle of flu and RSV season. When Adeline was getting ready for discharge from the NICU and I was trying to decide whether or not to return to work, I had a frank discussion with our team of neonatologists. They said if I could, stay home with her. Their recommendation was strict isolation during flu/RSV season during the first two years of life (except for doctors’ appointments & therapy). No daycare, only allow people around her who had been immunized with whooping cough, gotten their flu shot and limit visitors and germs. They even told us not to allow anyone except us kiss her until she was two (I made an exception for Nonna & PopPop).
They were less concerned about her being outside in nature. Even though we had to make a tremendous amount of sacrifices (financial, mental, emotional, etc.), I left my dream job to take care of Adeline, in isolation. Our lifestyle changed greatly and finances were much tighter, but I am grateful I was able to do that, as I know not all families can.
We took isolation seriously. I quit my job to care for my preemie. We left the house only for doctors’ appointments. We did not allow visitors. We did not attend family gatherings or holiday parties. We even had some people give us a hard time about this decision or even question it. This all made our first year home from the NICU very lonely. Our house was not full of visitors coming in and out to see the baby, surrounded by family and friends. It was depressing.
Early Intervention
Our first year home was filled with early intervention in our home and privately through our health insurance. Because of Adeline’s gestational age at birth, she automatically qualified for free early intervention services in our state called Infants and Toddlers. Infants and Toddlers came to our home and assessed her, and determined who her providers will be, and how often they will give her therapy. These types of services can also be delivered in a daycare.
 Adeline received services with a nurse, occupational therapist, physical therapist, special educator and eventually a speech language pathologist. This meant we had several appointments per week in the home and then in the private setting. At this age intervention is offered in a parent coaching style, so you are taught how to work on the skills at home, in the natural environment, during routines. We had lots to do at home. Luckily, since I was a special educator and early interventionist myself, this came natural to me. Through play I targeted a variety of skills, and we had a lot on our to-do list outside of the appointments. Adeline was also followed by a developmental pediatrician and was seen and assessed every three months as part of a NICU follow up clinic to keep an extra close eye on her skills and refer her to other providers if needed. We were referred to neurologist due to IVH (brain bleed) and tremors, so we were also seen every few months by them.
Adeline received services with a nurse, occupational therapist, physical therapist, special educator and eventually a speech language pathologist. This meant we had several appointments per week in the home and then in the private setting. At this age intervention is offered in a parent coaching style, so you are taught how to work on the skills at home, in the natural environment, during routines. We had lots to do at home. Luckily, since I was a special educator and early interventionist myself, this came natural to me. Through play I targeted a variety of skills, and we had a lot on our to-do list outside of the appointments. Adeline was also followed by a developmental pediatrician and was seen and assessed every three months as part of a NICU follow up clinic to keep an extra close eye on her skills and refer her to other providers if needed. We were referred to neurologist due to IVH (brain bleed) and tremors, so we were also seen every few months by them.
Doctor’s Appointments
 Our first year home was filled with doctor’s appointments. We thankfully qualified for in-home nursing, so weekly a nurse would come to get updates on Adeline, weigh her, check vitals, blood work, and more. This meant fewer visits to the pediatrician, which was so appreciated. Adeline was followed by a GI doctor, nutrition, surgery, and pulmonology monthly. She had several GI studies performed during her first year home as well: upper and lower GI studies, x-rays, and more.
Our first year home was filled with doctor’s appointments. We thankfully qualified for in-home nursing, so weekly a nurse would come to get updates on Adeline, weigh her, check vitals, blood work, and more. This meant fewer visits to the pediatrician, which was so appreciated. Adeline was followed by a GI doctor, nutrition, surgery, and pulmonology monthly. She had several GI studies performed during her first year home as well: upper and lower GI studies, x-rays, and more.
Hospitalizations
 When we walked out the doors of the hospital with our baby in her over-sized car seat, I never thought we’d be back inpatient. We would end up spending more time inside the hospital during her first year home than we did actually home. She ended up having three more surgeries that first year home, got a permanent feeding tube placed, had countless tests, and endured long inpatient stays due to feeding intolerance, growth issues, excessive vomiting, stooling blood, and more. We had to do an exploratory surgery in February because we could not figure out what was going on with her, and it turns out her intestines were twisted (intestinal malrotation), and blood flow was cut off to the intestines (volvulous). We could have lost her. Not long after that she was diagnosed with short bowel syndrome.
When we walked out the doors of the hospital with our baby in her over-sized car seat, I never thought we’d be back inpatient. We would end up spending more time inside the hospital during her first year home than we did actually home. She ended up having three more surgeries that first year home, got a permanent feeding tube placed, had countless tests, and endured long inpatient stays due to feeding intolerance, growth issues, excessive vomiting, stooling blood, and more. We had to do an exploratory surgery in February because we could not figure out what was going on with her, and it turns out her intestines were twisted (intestinal malrotation), and blood flow was cut off to the intestines (volvulous). We could have lost her. Not long after that she was diagnosed with short bowel syndrome.
PTSD
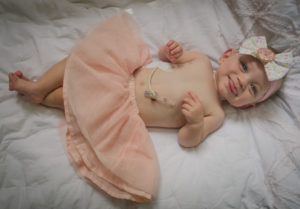 When you’re in it, sitting next to the isolette while your baby is struggling to survive, do you really have time to feel? Maybe I cried, freaked out at my husband, or worried constantly. But could I really process what was happening? I mean truly process. Did I really have the time to grieve? Or did she go blue and stop breathing in John’s arms, need to be resuscitated, and I coped with it by immediately taking an infant CPR class and going home to host my family for Thanksgiving? And then did I simply wake up the next day and deal with the next traumatic event? Even in the moments of joy we had in the NICU, could I experience that elation of being a mother without feeling a pit in my stomach or a pang in my heart?
When you’re in it, sitting next to the isolette while your baby is struggling to survive, do you really have time to feel? Maybe I cried, freaked out at my husband, or worried constantly. But could I really process what was happening? I mean truly process. Did I really have the time to grieve? Or did she go blue and stop breathing in John’s arms, need to be resuscitated, and I coped with it by immediately taking an infant CPR class and going home to host my family for Thanksgiving? And then did I simply wake up the next day and deal with the next traumatic event? Even in the moments of joy we had in the NICU, could I experience that elation of being a mother without feeling a pit in my stomach or a pang in my heart?
When we brought Adeline home, everyone (including myself) expected just to feel pure joy. But that was not the case. My mental health was suffering. I had difficulty sleeping, anxiety, and it was scary time. The likelihood of post-traumatic stress following childbirth, even in the absence of prematurity, is between 1.7–5.6%. PTSD following childbirth that results in a premature baby who spends at least 70 days in the NICU ranges from 23% to 59%. To add to that, how ill the infant was during the NICU hospitalization was directly related to mothers’ PTSD symptoms. The sicker the baby, the more likely they were to have PTSD. I see a counselor now and am receiving therapy which has been very helpful. I wish I’d done it sooner.
Joy
 When Hand to Hold asked me to write about this topic, I sort of hesitated. To be honest, I did not want to scare parents, since our first year home was not the best. But these stories need to be told as well, since it’s often reported throughout the preemie community and even media is that the premature baby “overcame” their early birth and are “completely fine” and you “would never know they were born prematurely.” For my family, that is not the case. Life after the NICU has been a struggle, with setbacks, successes and a lot of hard work.
When Hand to Hold asked me to write about this topic, I sort of hesitated. To be honest, I did not want to scare parents, since our first year home was not the best. But these stories need to be told as well, since it’s often reported throughout the preemie community and even media is that the premature baby “overcame” their early birth and are “completely fine” and you “would never know they were born prematurely.” For my family, that is not the case. Life after the NICU has been a struggle, with setbacks, successes and a lot of hard work.
My daughter is an amazing human being with a spirit that defies her reality. She has been our inspiration, the reason we fight, she constantly puts life into perspective, and has made me a better person. She inspires me to make the most of every moment, she inspires me to appreciate the tiniest things in life that mostly go unnoticed. She is a miracle, who has had to fight for her life more than once, has worked harder on everything she’s achieved, and yet her positivity is contagious. I strive to be more like her. Your first year home may have it’s challenges and you will wonder how you will survive, you will feel like it’s unfair (which it is), your heart will be break as your child suffers, you will feel isolated, and angry. All of those feelings are OK and let yourself feel them. But you gave birth to a warrior which means they’ve inherited that same spirit from somewhere.
So, let’s take a bit of advice from Poppy from Trolls,
“HEY!
I’m not giving up today
There’s nothing getting in my way
And if you knock knock me over
I will get back up again, Oh!
If something goes a little wrong
Well you can go ahead and bring it on
’Cause if you knock knock me over, I will get back up again”
— Trolls

